If you are the parent or guardian of a child on the autism spectrum, you know firsthand how frustrating and time-consuming it can be to get a diagnostic assessment for your child. The process often involves long wait times, multiple in-person appointments, and a lot of uncertainty. Thanks to recent advancements in telehealth technology, parents now have access to a faster and more convenient way to get their child assessed for autism.
Telehealth acceptance has been steadily increasing in recent years, with more patients and clinicians opting for virtual appointments over in-person visits. This trend has only accelerated during the COVID-19 pandemic, as many families were unable or unwilling to visit clinics in person and clinicians were prevented from having patients visit their clinics.
The benefits of telehealth go beyond convenience. Aided by innovative telehealth platforms and experienced clinicians, parents can now accelerate their child’s assessment when they use video conferencing and other telehealth tools from their home. For example, if the parent and child are comfortable doing so, a recording of the child’s behavior can be shared with a trained, diagnostic clinician. This alternative way of pursuing a diagnostic evaluation can be a faster and more efficient than traditional in-person assessments, the standard of care that families have been following for decades.
What is NODA?
NODA™ stands for the Naturalistic Observation Diagnostic Assessment and is an evidence-supported hybrid (synchronous and asynchronous) telehealth platform that supports families seeking faster, quality diagnostic assessments for autism, particularly those living in underserved areas. What has emerged is potentially the most prospectively research-based telehealth method to help young families who suspect their child should be evaluated for autism.
How NODA Works:
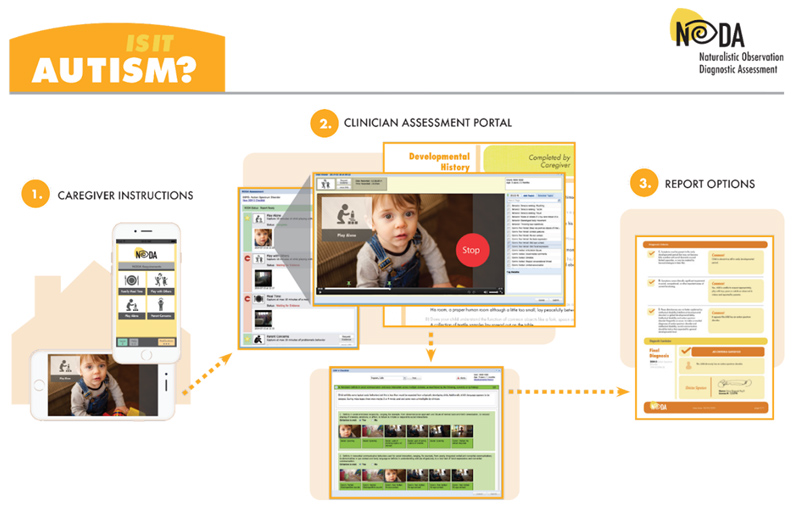
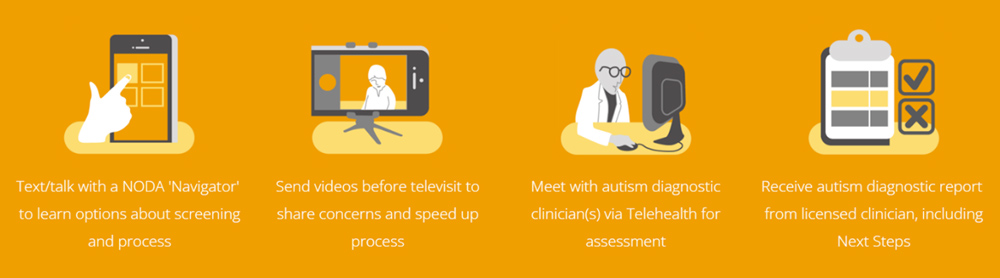
- Parents download the NODA app and set up a secure account. Then, the NODA app prompts them to complete a diagnostic history questionnaire and then record and upload short videos of their child in various situations at home: mealtime, bedtime, playtime with others, and playtime alone.
- Experienced clinicians then view the videos, tag behaviors relevant to a diagnosis of autism, and NODA organizes these tags according to the DSM-5 and virtually meets with the family (occasionally more than once)
- The clinician renders a diagnosis and provides a complete diagnostic assessment report to the patient’s family.
What Parents Can Expect:
There are a few steps parents can expect when they use NODA to get their diagnostic assessment done:
- Usually after the child has been screened “positive” by their pediatrician or other referring source, the family can register on the NODA app where they fill out an adaptive behavior assessment and development history questionnaire. They then follow instructions to capture and share clinically-guided video examples of their child’s behavior in and around their home.
- A licensed NODA diagnostic clinician who is already trained to assess autism in-person will receive the in-home behavior specimen collection (videos and developmental history) via their secure access to the NODA Telehealth platform. During their analysis, this clinician may interact with the family through the NODA app if more data is requested. The NODA clinician analyzes each video sample and clinically tags all atypical and typical behaviors based on his/her clinical judgment, and the platform correlates these tags to DSM-5 criteria if applicable.
- (Since 2021) The NODA Clinician will then use a novel real-time telehealth tool that enables him/her to interact with families via video chat, so he can gather more history and potentially analyze / archive additional naturalistic behavior data. At this juncture, the clinician can usually educate families about their findings and recommended next steps.
- The NODA clinician then can provide a thorough report of findings via a diagnostic assessment report that the families can access from their NODA app. These reports are instrumental to qualify the child for intervention services if warranted.
With family consent, referring providers, insurance payors, and treatment clinicians can be included in the distribution of this diagnostic assessment report. A NODA report can also provide a list of local or online treatment centers, which could jumpstart the process of matching a diagnosed child with a specific treatment provider.
Any telehealth program used to deliver healthcare for any health condition operates more effectively when the clinicians make their clinical decisions with the same degree of confidence relative to an in-office visit. Several prospectively-executed research studies funded by the National Institutes of Health confirm that clinicians have a high level of confidence when using NODA to evaluate patients. Most families do not consider a virtual exam as inferior to an in-office visit. As one family described their experience to one of the clinics that now uses NODA for all diagnostic assessments during and post-pandemic, “We just got a diagnosis from the Southwest Autism Research & Resource Center (SARRC). The wait time was really short, everything was done over the phone or on the computer, and everyone I spoke with was really pleasant to work with. We were very happy with them!” That is the goal for any telehealth technology provider, especially when it involves a more efficient way to collect and analyze data for one of the most important moments in finding life-changing solutions for their child.
By following the NODA protocol, families can save time and reduce stress by avoiding long travel times and waitlists associated with in-person assessments. NODA also allows clinicians to perform assessments while they are traveling, after clinic hours, on weekends, and it has the added benefit of clinicians observing the individual in the patient’s natural setting when behaviors occur and/or via a videochat. This new way of gaining evidence for a diagnostic assessment has the potential to revolutionize the way autism diagnoses are made and provide families with earlier access to intervention services.
For more information, visit https://behaviorimaging.com/NODA.
References
Matthews NL, Abowd GD, Rozga A, Fein DA. Medical and Healthcare Applications. In: O’Brien HL, Rogers WA, Fisk AD, editors. Handbook of Human-Computer Interaction in Healthcare. Springer; 2010. pp. 563–580.
Nazneen N, Matthews N, Smith CJ, Rozga A, Abowd GD, Oberleitner R, Arriaga RI. Supporting in-home collection and sharing of behavior specimens for diagnostic assessment of children with autism. J Biomed Inform. 2015 Aug;56:147-57. doi: 10.1016/j.jbi.2015.05.006. Epub 2015 May 18. PMID: 26002838; PMCID: PMC4541279.
Oberleitner R, Ball J, Gillette D, Naseef R, Stamm BH. Technologies to lessen the distress of autism. Journal of Aggression, Maltreatment & Trauma. 2006 Jan 1;12(1-2):221-42.
Smith CJ, Rozga A, Matthews N, Oberleitner R, Nazneen N, Abowd G. Investigating the accuracy of a novel telehealth diagnostic approach for autism spectrum disorder. Psychol Assess. 2017 Mar;29(3):245-252. doi: 10.1037/pas0000317. Epub 2016 May 19. PMID: 27196689; PMCID: PMC5116282.
Southwest Autism Research Center (Phoenix, AZ) Letter from the President / CEO – February, 2023.
NODA – Founded by Parents, for Parents
The origins of researching autism diagnosis and telehealth may go back to 1995, when Medical device industry executive and dad Ron Oberleitner and his wife Sharon began “losing our son” (15-month-old Robby) is the only way they could describe it.

Robby at 7 years, after being diagnosed
with Profound Autism at 3 ½ years.
Robby’s body was still intact and growing, but 180 degrees different from his two older brothers’ development years earlier. Robby started losing the few FIRST words he had learned (flower, dada, mama), and instead, started to shriek, tantrum and cry for hours on end seemingly every day. He stopped eating and began to pick at his food instead, and at a moment’s notice, may run out of the house naked to go… anywhere. The changes to Robby affected him on a daily basis and the discomfort could last several hours, until he passed out (it seemed). Robby’s parents took him to their family pediatrician several times after witnessing Robby’s increasingly distressing and indescribably torturous behavior. That overlapped with a decline in his ability or interest to interact with his mom and dad. Eventually his interaction with others dissolved as though it was never there. To anyone who observed Robby at that time, he seemed to be in constant pain and discomfort, and in his own world.
As it would happen with any family, the Oberleitners would take trips so that Robby could be evaluated by different “medical specialists” with whom they shared their concern about Robby’s erratic behavior and sleeplessness. As Robby’s situation grew increasingly concerning, Ron’s work responsibilities raised an interesting thought. Ron’s position included oversight of novel health care initiatives that studied how surgery patients could safely be evaluated post-operatively from the safety of their home via Skype or secure videoconferencing. Patients could also get tertiary expert opinions by forwarding photos of post-operative wounds. While carrying out his job responsibilities, Ron was struck by the thought that this technology could be implemented for his and other families who, along with their children, were experiencing an increasingly difficult situation. There was always a hounding thought, “Why aren’t we doing this to help doctors see what’s happening in our home?”
Robby was ultimately diagnosed with autism in 1996. That led directly to the formation of Princeton Autism Technology by Ron and Sharon Oberleitner. The family formed a nonprofit that collaborated with autism doctors to assess if and how telehealth images could expedite and improve access to healthcare for families with autistic children. Several pilot studies with interested autism centers showed the promise of what parents can provide if asked to send video data, and agencies including NIH, Dept of Defense, and private autism foundations started funding pilot projects.

The Oberleitners at the annual autism research meeting (INSAR) in Rotterdam, Netherlands in 2018
After developing telehealth applications for treating children with autism showed great promise to help get their own son treatment for his challenging behaviors, Ron and Sharon organized a multi-disciplinary team of diagnostic clinicians, academic researchers, technologists, parents of children with autism, and other medical device industry veterans to create a telehealth platform to enable what is now known as the Naturalistic Observation Diagnostic Assessment (NODA™). What has emerged is the most prospectively research-based telehealth method to help young families who have suspect that their child should be evaluated for autism.
NODA was developed in conjunction with Georgia Tech University, Southwestern Autism Research and Resource Center (Phoenix, AZ), and several other leading academic research partners, and is proving conclusive for over 88% of children when compared to the conventional In Person Assessments (IPA).
Since the pandemic, NODA has helped thousands of families connect remotely to diagnostic doctors, and there are now over 1,000 clinicians who’ve received online training for NODA, and more than 40 clinics in 20+ states in 5 countries who have incorporated NODA into their practice. The app has been translated into Japanese, Sweden, Arabic (Saudi Arabia), and Spanish for international uses and underserved US populations.